According to the World Health Organization (WHO), obesity is defined
as “abnormal or excessive fat accumulation that presents a risk to
health”.1 In contrast to the view that obesity only
represents a risk factor for diseases, the World Obesity Federation
declared obesity itself as a chronic relapsing progressive disease.2
In current guidelines, diagnosis of obesity and treatment decisions
are based on a body mass index (BMI) ≥30kg/m², despite the inability
of BMI to accurately predict cardiometabolic risk or to define total
and central abdominal fat mass.3 At any given BMI, the
variation in comorbidities and health risk factors is remarkably high.3
Obesity may be considered a consequence of the interaction of
different disease-causing factors. Such obesogenic factors include
biologic (e.g. age, sex, genetics), society (e.g. work place, mode of
transportation), behavior modifying (e.g. family, eating culture,
friends) and environmental factors (e.g. availability and
accessibility of energy-rich food, low requirements for physical
activity).4 Many of these obesogenic factors cannot be
actively changed which supports the view obesity is a disease not a
decision. Together they can promote weight gain and maintain higher
BMI even against targeted weight-loss attempts. Defining obesity as a
disease would have a strong impact both on the individual in terms of
improving self-esteem and reducing stigma, and on wider society in
terms of increasing awareness amongst both health care professionals
and politicians.
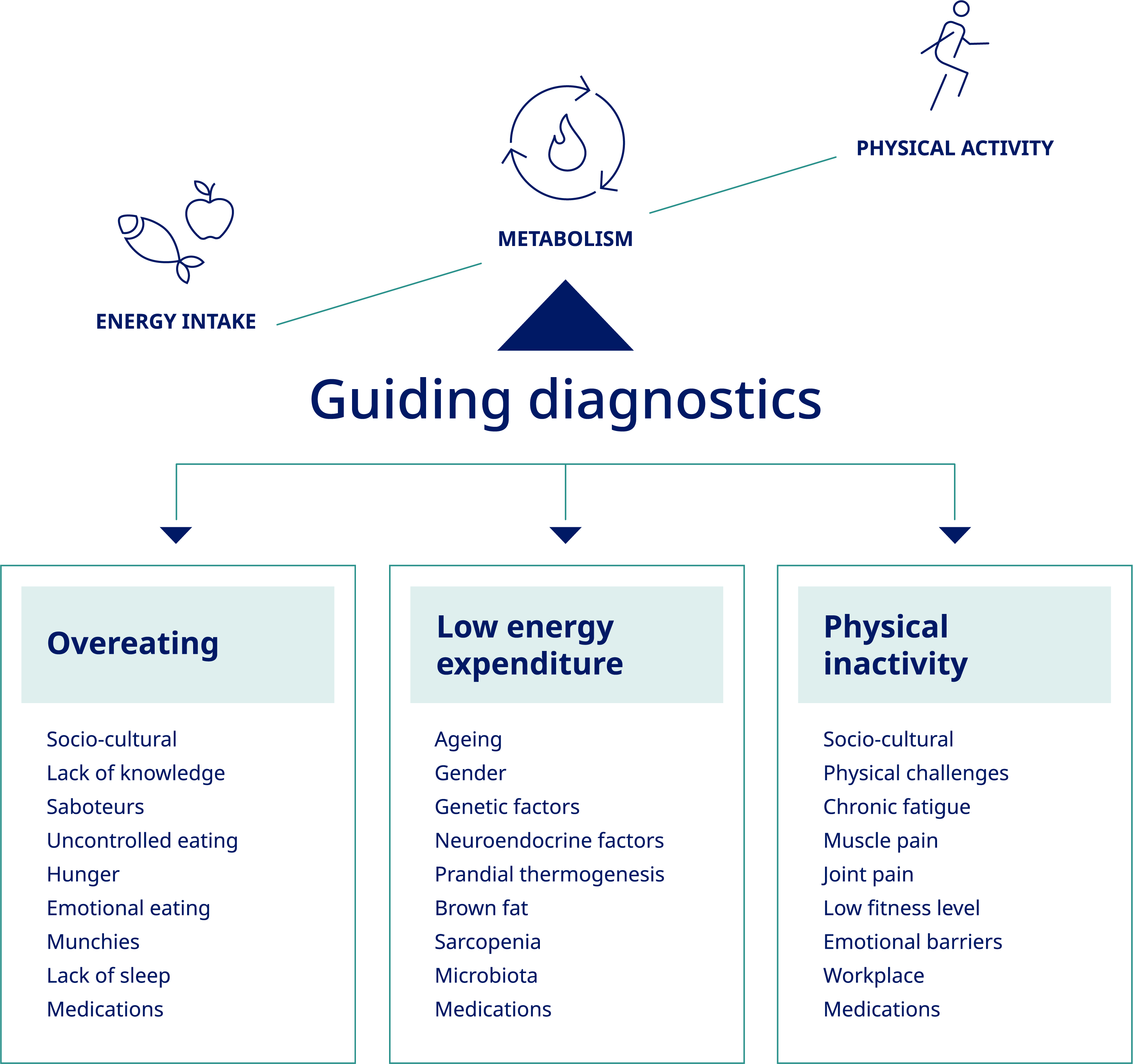
Health care professionals initially ask people with obesity about
root causes and lifestyle factors (Figure 1) that may have led
to development of unhealthy body weight and there will be a physical
examination including measurements and blood tests.
Assessment of family and health history. Because obesity is
considered a heritable disease, people with obesity will be asked
about the body weight of parents, siblings and other relatives. There
will also be a review of body weight history, weight-loss attempts and
success, physical activity and exercise habits, eating patterns,
satiety and appetite control, medications, stress levels, sleep and
work patterns.
Physical examination. In addition to measurements of body
weight, height, waist and hip circumferences, heart rate, blood
pressure and body temperature are checked and the heart, lungs,
abdomen and joints are examined. With the weight and height data, the
BMI can be calculated to formally establish the obesity diagnosis and
to stratify treatment.
BMI should be checked at least once a year to determine overall
health risks, define treatment goals and inform strategies for weight loss.
Central fat distribution - which is associated with increased risk
of cardio-metabolic disease- can be estimated by the waist
circumference. For women, a waist circumference of more than 88 cm and
for men more than 102 cm increases this risk. Based on these physical
examination, further tests, such as ultrasound or an electrocardiogram
may be recommended.
Body composition. A higher BMI can be misleading if people have
large muscle mass. Therefore, body composition - fat, muscle and water
components, are assessed by bioimpedance analyses or dual X-ray
absorptiometry measurements. These analyses may provide important
guidance for types of weight loss intervention because it is a more
important treatment goal to reduce fat mass rather than total body mass.
Blood tests. Blood tests should be performed at the first visit
to check for endocrine disorders that may cause obesity including
hypothyroidism and hypercortisolism. In addition, blood tests are
required to diagnose other obesity-related diseases or risk factors,
therefore parameters of lipid and glucose metabolism, chronic
inflammatory states as well as kidney and liver function tests should
be performed.
In some people, obesity may not cause any health impairments whereas
in others it may cause metabolic issues (e.g. type 2 diabetes,
dyslipidemia, fatty liver disease), cardiovascular diseases (e.g.
hypertension, myocardial infarction, stroke), osteoarthritis, back
pain, asthma, depression, cognitive impairment and even some types of
cancer (e.g. breast, ovarian, prostate, liver, kidney, colon).4
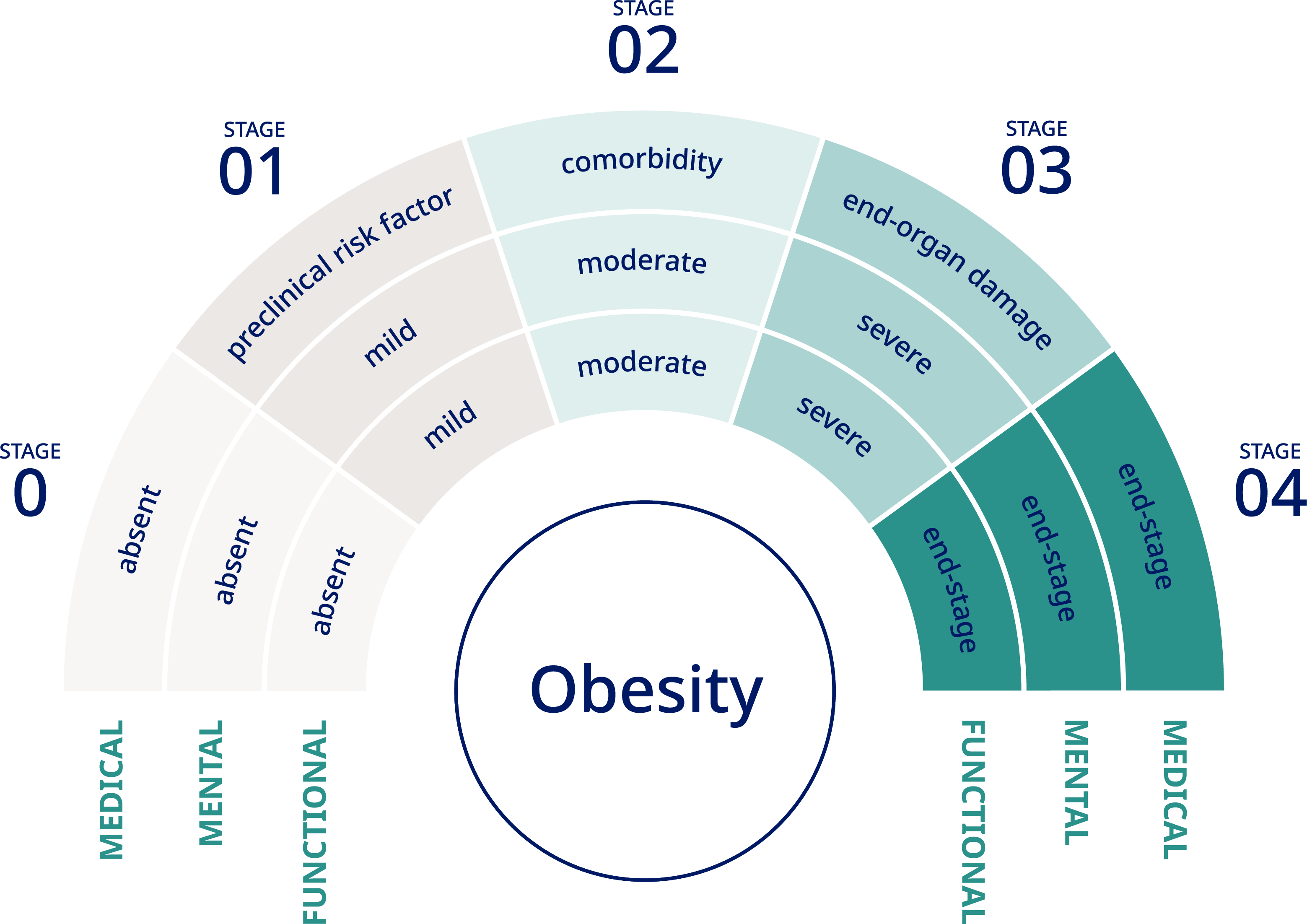
BMI and waist circumference do not always reflect adverse
obesity-associated health outcomes and the Edmonton Obesity Staging
System (EOSS) has been developed as a five-stage system of obesity
classification that takes account of metabolic, physical and
psychological impairments (Figure 2). This system is intended
to address the need for a more individualized definition of obesity
and improve treatment decisions.5
Careful obesity diagnostics are the most important prerequisite to
determine whether and how much weight a person with obesity should
lose and what health conditions or risks are already present. Obesity
diagnostics should identify individual predominant obesity causes and
guide treatment decisions.